Functional Analysis and Surgical Planning
Jess Snedeker (ETH/UZH)
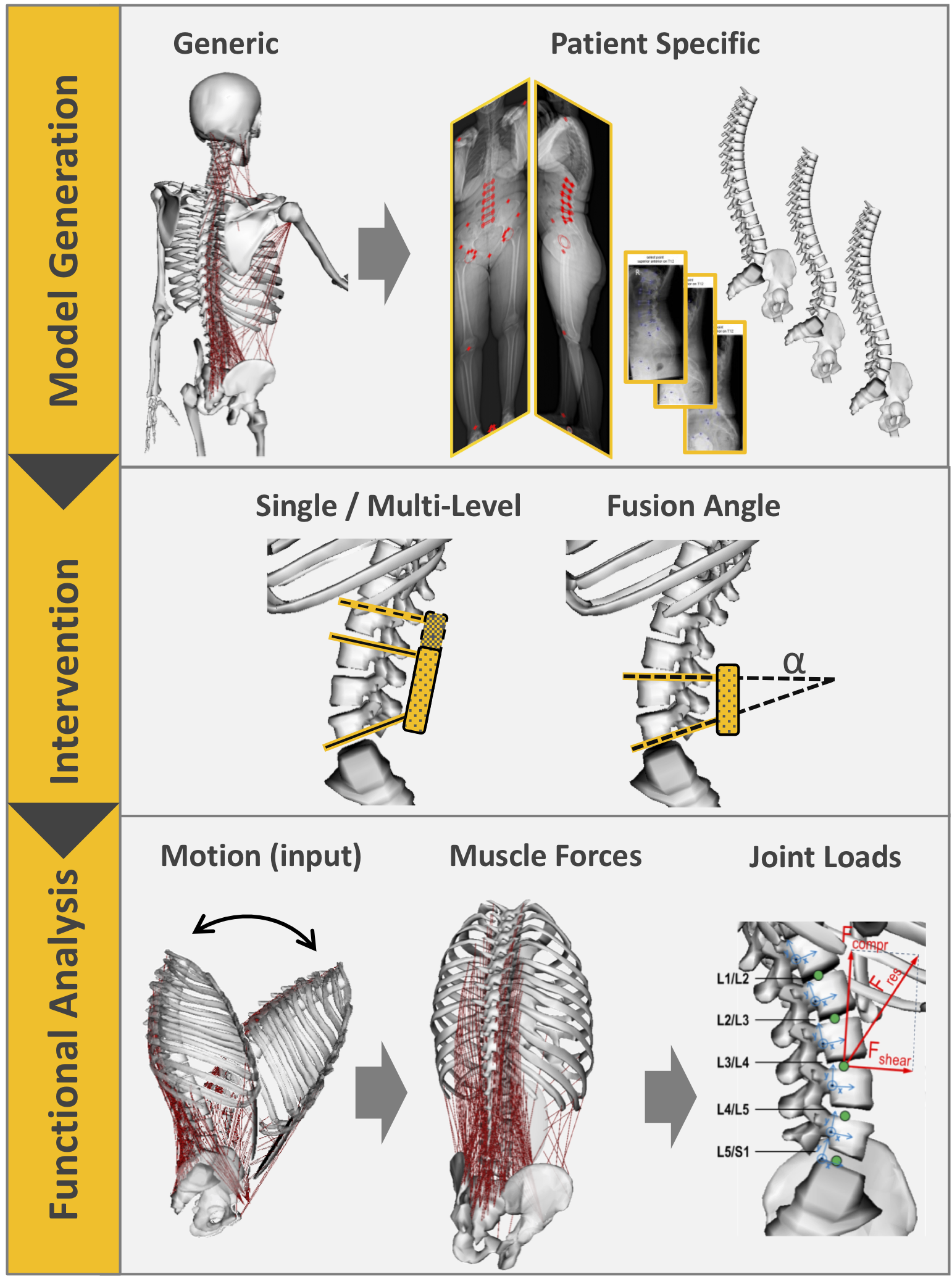
Patient-specific anatomic geometries and structural information obtained from work package 1 will be used for the automatic creation of personalized functional models. The analysis of these models will allow developing optimal patient-specific operation planning, as well as making outcome prediction possible. Depending on the application case, multi-rigid body (MRB) musculoskeletal models, finite element (FE) models, and/or anatomical functional models will be employed and combined. This will allow evaluating joint and muscular loads, structural loads in biological tissues (e.g. bones, intervertebral discs, nerves) and devices interacting therewith (e.g. pedicle screws, fusion rods, intervertebral cages), as well as the spatial distribution of functional properties obtained from patient imaging data. The created models can then be used to perform functional analysis of specific interventions and the possible treatment options can be rated through a quantitative evaluation of the results obtained with varying surgical parameters (e.g. screw position, longitudinal rod position/curvature, strategy for nerve decompression).
The output of the intervention modelling and analysis will supply surgeons with standardized quantitative information regarding various aspects of the intervention or patient outcome, saving operating time and increasing accuracy during realization of the surgical plan. While the clinical decision-making process itself remains the same as in traditional planning of spine surgeries, it is enriched with extra information on functional surgical outcome that will ultimately support spine surgeons in identifying favorable surgical parameters. The selected patient-specific surgical parameters will be forwarded to work package 3 to ensure precise implementation of the chosen protocol and navigation map by intraoperative holographic navigation.